- Home
- Common Foot Problems
- Cuboid Syndrome
Cuboid Syndrome
Written By: Chloe Wilson BSc(Hons) Physiotherapy
Reviewed By: FPE Medical Review Board
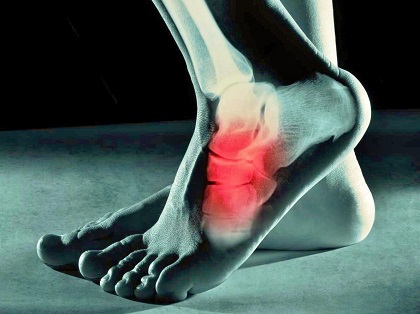
Cuboid Syndrome is a common cause of lateral foot pain i.e. pain on the outer side of the foot.
Whilst fairly simple to treat, it is often misdiagnosed so symptoms can last for a long time. It particularly affects athletes such as ballet dancers and runners.
The condition develops when the cuboid bone, one of the small bones in the foot, subluxes i.e. partially dislocates.
This may happen suddenly due to an injury such as an ankle sprain, or develop gradually overtime from repetitive tension through the bone and surrounding structures.
Here, we will look at the common causes of cuboid syndrome, how it presents, diagnosis and the best treatment options.
What Is Cuboid Syndrome?
The cuboid is one of the small bones
on the outer side of the midfoot. It attaches to the heel bone
(calcaneus) via a number of strong ligaments and a joint capsule forming
the calcaneocuboid joint.
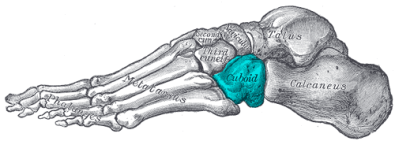
Trauma to the foot, be it a sudden injury or gradually repetitive forces may damage the supporting soft tissues causing the cuboid bone to move out of its usual position. It can then act like a block, limiting the movement of the surrounding bones in the foot.
Other terms commonly used are cuboid subluxation, blocked cuboid, dropped cuboid, lateral plantar neuritis and cuboid fault syndrome.
What Causes Cuboid Bone Pain?
There are three main causes of Cuboid Syndrome:
1. Ankle Injury
The most common injury that causes cuboid subluxation is an inversion sprain of the ankle. This is when the foot and heel bone are forced inwards while the cuboid is forced outwards.
This inwards twisting damages the soft tissues which support the bone in place causing it to partially dislocate. In this instance, cuboid pain usually comes on suddenly.
2. Repetitive Strain
Another common cause of cuboid syndrome is repetitive strain. The peroneus longus muscle runs down the outer side of the lower leg attaching on to the outer side of the foot. Tension placed through this muscle from repetitive activities such as ballet (pointing), jumping and running may cause excessive traction on the cuboid bone causing it to sublux.
In this case, symptoms come on gradually over time and often fluctuate.
3. Altered Foot Biomechanics
Studies have shown that a majority of people suffering from cuboid subluxation have over-pronated feet i.e. flat feet.
Symptoms of Cuboid Subluxation
Common symptoms of Cuboid Syndrome include:
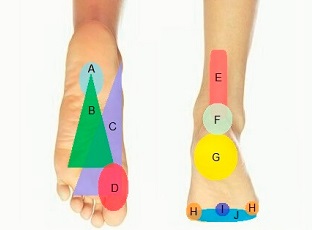
- Lateral Foot Pain: pain down the outside of the foot which can refer across the foot and to the ankle and toes
- Pain Worse With Activity: Pain is usually worse when weight-bearing particularly first thing in the morning, on uneven ground, quickly changing direction, jumping or hopping and symptoms tend to ease with rest
- Difficulty Walking: Walking may be difficult and people with cuboid subluxation often walk with a limp in an attempt to keep their weight of the outer foot
- Tenderness & Swelling: The bone is usually tender to touch and the area may be slightly red and swollen
- Weakness: The foot may also feel weak, especially during the push-off phase of walking, running and jumping
Diagnosing Cuboid Subluxation
Diagnosing a subluxed cuboid can be difficult and cuboid syndrome is often misdiagnosed. Imaging studies such as x-rays, MRIs and CT scans often fail to show cuboid subluxation but they can be useful for ruling out other causes of pain.
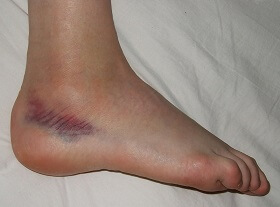
There is no conclusive cuboid syndrome test but your doctor will usually assess to see if there is pain and stiffness on palpation of the bone (when they press firmly on the cuboid through the sole of your foot).
They may also move your foot inwards and outwards to see if that elicits pain or get you to try and hop.
Some health professionals may use the midtarsal adduction test or midtarsal supination test to assess for the condition.
Cuboid Syndrome often goes undiagnosed with ankle sprains. If symptoms continue more than three months following an inversion sprain, cuboid subluxation should be considered.
Other things that cause similar symptoms to cuboidsyndrome are:
- Jones Fracture: a break in the 5th metatarsal bone
- Ankle Sprain: overstretching or tearing of one of the ankle ligaments
- Peroneal Tendonitis: inflammation of one of the tendons on the outer foot
How Do You Treat Cuboid Syndrome?
The best treatment options for Cuboid Syndrome are:
1. Exercises
Cuboid syndrome exercises are a vital part of treatment and should incorporate a selection of:
- Movement Exercises: foot mobility and stretching exercises for cuboid syndrome help to not only reduce any foot or ankle stiffness but to also regain any lost movement
- Strengthening Exercises: help to improve strength and endurance in the foot and ankle muscles
- Stability Exercises: help to improve balance and ankle stability to reduce the risk of further foot and ankle injuries such as ankle sprains in the future. A simple one to start with is standing on one leg and closing your eyes.
Cuboid syndrome exercises should be started as soon as possible and performed daily, gradually progressed as symptoms allow and continued until full function of the foot is restored.
The quicker treatment commences following a cuboid subluxation, the quicker full function will be restored. Chronic (long-term) cases, will take longer to heal.
2. Manipulation
The most successful treatment for a subluxed cuboid is to have the bone relocated back into its proper position.
A health professional such as a doctor, physical therapist or podiatrist will perform a manipulation, which is a high velocity (quick) small amplitude thrust to the cuboid bone to relocate it. This should only ever be carried out by a trained professional. The symptoms of cuboid syndrome will usually settle immediately if the manipulation is done correctly.
Manipulations for cuboid syndrome are not a suitable treatment if you suffer from gout, bone disease, fracture, rheumatoid arthritis or nerve or vascular problems.
Following successful manipulation, other cuboid syndrome treatments will help to keep the bone in the correct position and to treat any lingering symptoms.
3. Cuboid Syndrome Taping
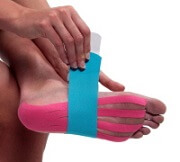
Taping can be a useful cuboid syndrome treatment tool. Taping of the foot and ankle is often used to support and stabilize the bones in the foot with cuboid syndrome. Medical tape is used to support and stabilize the bones in the foot and hold the cuboid in place while the surrounding soft tissues heal.
Correct taping for cuboid syndrome should allow you to walk without pain. Your physio should be able to teach you how to apply cuboid syndrome taping correctly.
4. Ice Therapy
Ice therapy can help to reduce pain and inflammation as part of your cuboid syndrome treatment. Place an ice pack or bag of frozen veg wrapped in a tea towel over the outside of the foot for ten minutes at a time.
To find out more visit the Ice Therapy section including how to safely and effectively use ice.
5. Rest
Rest from aggravating activities is a really important part of cuboid syndrome treatment. In most cases, 6-8 weeks of rest is recommended before returning to sports or any challenging activities. In some cases, people are advised to use crutches for a short period of time to keep weight off the subluxed cuboid completely.
6. Orthotics

Specially designed shoe inserts can be a helpful part of cuboid syndrome treatment. If over-pronation of your foot (i.e. flat feet) is thought to have been a contributing factor to developing cuboid syndrome, you should be given orthotic insoles to wear in your shoes to correct your foot position to relieve tension on the peroneus longus tendon and support the foot bones and arches.
7. Cuboid Wedge
You may also be given a small foam wedge to wear in your shoe which helps to support the cuboid bone in the correct position.
Interesting Stats
- 80% of people with cuboid subluxation have over-pronated feet
- Cuboid Syndrome accounts for 4% of foot injuries in athletes but 17% of foot injuries in ballet dancers
- 6.7% of ankle inversion sprain sufferers also have a subluxed cuboid
- The cuboid bone rotates approximately 25 degrees when inverting and everting the foot (turning it inwards and outwards)
What Else Can Help?
There are a number of other causes of pain on the outside of the foot other than Cuboid Syndrome.
If this is not sounding like your problem, visit the side foot pain or foot pain diagnosis sections for helping working out what is causing your pain.
You may also be interested in the following articles:
- Pain On Top Of Foot
- Foot Arch Pain
- Nerve Pain In The Foot
- Foot & Ankle Stretches
- Swollen Feet & Ankles
- Foot Numbness
- Foot Lumps & Bumps
*Stats Source: Sports Health Journal
Related Articles
Page Last Updated: 26th November, 2024
Next Review Due: 26th November, 2026