- Home
- Common Foot Problems
- Tendonitis Guide
- Achilles Tendonitis
Achilles Tendonitis Treatment
Written By: Chloe Wilson BSc(Hons) Physiotherapy
Reviewed By: FPE Medical Review Board
Achilles tendonitis treatment aims to reduce the pain, inflammation and stiffness so commonly associated with achilles tendonitis.
The achilles tendon is the largest and strongest tendon in the body but it is prone to damage by overuse, inflammation and degeneration.
Tendonitis is the most common cause of achilles heel pain. It can take months to recover fully, making early, effective achilles tendonitis treatment vital. Achilles tendonitis is one of the most common types of foot tendonitis.
Here we will look at the causes, symptoms and different types of achilles heel pain, as well as a whole range of achilles tendonitis treatment options including prevention strategies the problem from coming back.
What Is Achilles Tendonitis?
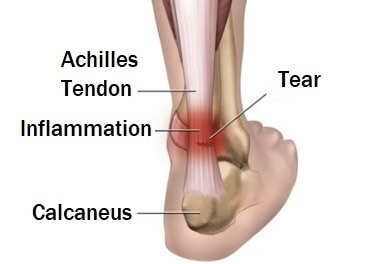
The achilles tendon is found on the back of the lower leg joining the two calf muscles, gastrocnemius and soleus, to the heel bone aka calcaneus.
The tendon is approximately six inches long. The muscle fibres run down the back of the calf, twist round through ninety degrees and then insert into the heel.
The achilles tendon is extremely strong and can withstand forces up to twelve times bodyweight, but it is not very flexible, making it prone to damage.
It has an hour-glass type shape being wider at the top and bottom than in the middle.
Achilles heel pain most commonly develops due to repetitive stress through the tendon rather than from a specific injury.
The tendon becomes fatigued and is unable to heal properly from the repetitive micro-trauma. The collagen fibres, that should be nicely aligned, begin to weaken and the crosslink’s between them break. The result is microscopic tears in the tendon.
What Causes Achilles Tendonitis?
Common causes of achilles tendonitis include:
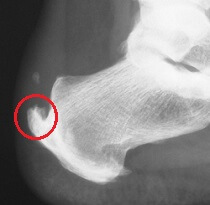
- Heel Bone Spurs: Bone spurs develop when the body lays down extra
layers of bone in an attempt to protect itself from repetitive friction
or stress. Burn spurs commonly develop at the back of the heel from wearing shoes
that are too tight, often known as a “pump bump” or due to muscle
tightness. The bone spur rubs on the tendon leading to damage
and resultant tendonitis
- Muscle Tightness or Weakness: Tightness and weakness in the calf muscles results in extra tension and stress on the tendon which can cause achilles tendonitis
- Altered Foot Biomechanics: Abnormal foot position such as over-pronation, flat feet and joint stiffness puts more strain on the tendon increase the chance of achilles damage and resultant tendonitis
- Sudden Increase in Activity Levels: changes in the intensity, frequency or amount of exercise can cause tendonitis if the achilles is suddenly overworked
Where Do You Get Achilles Tendonitis?
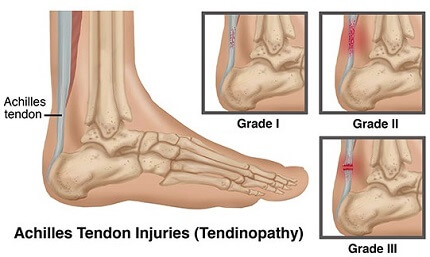
Achilles tendonitis can develop in two places:
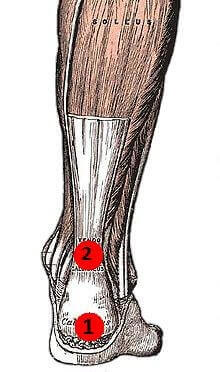
- Insertional Tendonitis: This occurs at the bottom of the heel where the tendon attaches to the heel bone. This can affect anyone, whether they have an active or sedentary lifestyle. It can be accompanied by extra bone growth, known as bone spurs, on the heel which exacerbates the problem.
- Non-Insertional Tendonitis: This occurs in the middle of the tendon, about two to four centimetres up from the ankle, where the tendon is at its narrowest and has the worst blood supply. Non-insertional tendonitis tends to affect athletes and younger individuals.
Effective achilles tendonitis treatment should target the specific location of the problem. Sometimes, the tendonitis can progress to tendonosis where there is no sign of inflammation, but instead degenerative lesions are seen.
Achilles Tendonitis Symptoms
The three main symptoms most commonly associated with achilles tendonitis are:
- Heel & Calf Pain: This tends to be over the area of tendonitis and sometimes radiates out to the calf region and heel. Achilles tendonitis pain is usually worst first thing in the morning or after prolonged rest. The first few steps you take are often agony but the pain subsides after a few minutes as the tendon relaxes out.
In the early stages, achilles heel pain tends to follow strenuous activity, but with more chronic (long-term) conditions, pain can occur during all activity and even sometimes at rest
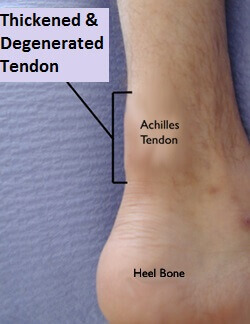
- Tendon Thickening: You can often feel a lump in the affected area of the achilles tendon which can be painful to touch. The lump varies in size depending on the severity of the achilles tendonitis and the location
- Stiffness: the ankle and calf often become tight and stiff with achilles tendonitis, limiting foot movement. Again, this tends to be worst after prolonged rest and eases with gentle movement
How Is Achilles Tendonitis Diagnosed?
Your doctor can usually make an accurate diagnosis of achilles tendonitis from what you tell them and from examining your leg.
The doctor will get you push your foot down (plantarflexion) against resistance or rise up onto your tiptoes when standing. If this is painful, it indicates tendonitis. If you are unable to do this, it indicates a more severe injury, most likely a rupture of the tendon.
An x-ray may be performed if a calcaneal bone spur is suspected.
This helpful video from the American Academy of Orthopedic Surgeons looks at what happens if the tendon does completely rupture.
#CommissionEarned from Amazon on qualifying purchases
Achilles Tendonitis Treatment
There are a number of different achilles tendonitis treatment options. Their main aims are to reduce the inflammation and irritation to the tendon. The best treatments for achilles tendonitis are:
1. Rest
Adequate rest is the most important part of achilles tendonitis treatment. The tendon must be given time to recover. Try as much as possible to avoid activities which provoke your symptoms. In severe cases, a walking boot or crutches may be required for a few weeks to completely rest the tendon.
2. Orthotics
Wearing simple heel pads in your shoes can reduce the tension on the tendon - a simple yet effective Achilles tendonitis treatment. If altered foot biomechanics is thought to be contributing to your problem, an Orthotist can give you appropriate insoles to help correct the problem.
3. Ice
Using ice can help to reduce the pain and inflammation associated with tendonitis. However, if it is used incorrectly, it can actually make things worse. Visit the Ice Therapy section to find out how to apply ice safely and effectively.
4. Physiotherapy
Physiotherapy is a very important part of achilles tendonitis treatment. As well as giving you an exercise programme, your physiotherapist may carry out deep transverse frictions. This is a specific type of massage involving friction being applied transversely over the site of injury. I have had good success with patients using this. It may be followed by ultrasound treatment. Both help to improve blood flow to the area and realign the damaged fibres to promote healing.
5. Low Impact Exercises
Switching to activities such as swimming and cycling put much less strain on the achilles tendon than high impact activities like running and jumping.
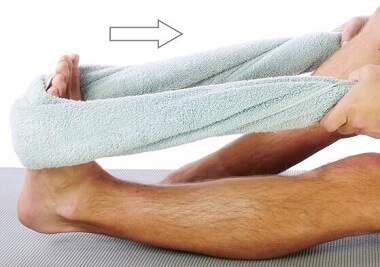
6. Stretches
Stretches should always be a part of achilles tendonitis treatment. If the calf muscles are tight, stretches will help to reduce the tension on the tendon.
However, stretches should not be performed until resisted plantarflexion e.g. rising up onto your tiptoes, is pain-free otherwise further damage may occur.
Visit the calf stretches section to find out how to safely and effectively stretch the two calf muscles
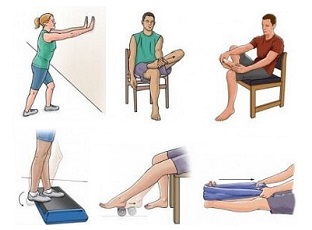
7. Strengthening Exercises
Strengthening exercises are also an important part of achilles tendonitis treatment. By strengthening the calf muscles you can really help reduce the strain on the tendon.
Visit the calf workout section for a whole range of exercises to strengthen the calf muscles as part of your achilles tendonitis treatment.
8. Eccentric Exercises
If the condition has progressed to tendonosis, eccentric exercises over a course of three to four months are one of the most effective treatments. Eccentric exercises are when you work the muscle as it is relaxing and lengthening, rather than as it is contracting and shortening.
It is thought that they work by increasing the tensile strength and the length of the tendon, and causing hypertrophy where the tissues increase in volume, and she always be included as part of achilles tendonitis treatment.
9. Medication
Non-steroidal anti-inflammatories such as ibuprofen and naproxen can help reduce achilles pain, but will not reduce the thickening in the tendon caused by degeneration so this achilles tendonitis treatment must be carried out in conjunction with others.
Many people find that certain creams and gels can be a really useful tool with achilles tendonitis treatment. Simply rub them in to the skin around the achilles tendon and they can reduce pain and inflammation. The most popular ones are Arnica and Tiger Balm.
10. Injections
Cortisone injections can be used to reduce pain and inflammation as part of achilles tendonitis treatment. The steroid tends to be peppered around the tendon, rather than inserted directly into the tendon to reduce the risk of the tendon rupturing.
Care must be taken for a few days following injections as they can temporarily weaken the tendon. You can find out more about steroid injections and how they work on our sister site.
How Long Does It Take To Recover From Achilles Tendonitis?
Recovery from achilles tendonitis unfortunately tends to be slow. This is because the blood supply to the tendon is poor, reducing the circulation of the necessary oxygen and nutrients for healing.
It usually takes between three and six months of consistent achilles tendonitis treatment to fully recover. It is important to rest from aggravating activities to allow the tendon to heal.
What Else Can Help?
Achilles tendonitis treatment should be started as soon as possible to prevent the condition getting worse.
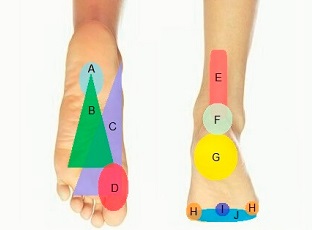
Tendonitis can occur in a number of locations around the foot, with the most common types of foot tendonitis being:
- Peroneal Tendonitis: Causes pain down the back and outer side of the foot
- Posterior Tibial Tendonitis: Causes pain on the inner side of the foot
- Extensor Tendonitis: Causes pain on top of the foot
- Tibialis Anterior Tendonitis: Causes pain on the front of the ankle
Achilles tendonitis is one of the most common causes of pain at the back of the foot, but there are other possible causes of causes of heel pain and heel lumps that you may be interested in.
You may also be interested in the following articles:
- Pain On Side Of Foot
- Foot Arch Pain
- Nerve Pain In The Foot
- Foot & Ankle Stretches
- Swollen Feet & Ankles
- Foot Numbness
- Foot Lumps
Related Articles
Page Last Updated: 02/28/24
Next Review Due: 02/28/26