- Home
- Diagnosis Guide
- Foot Lumps
- Piezogenic Papules
Piezogenic Papules
Written By: Chloe Wilson BSc(Hons) Physiotherapy
Reviewed By: FPE Medical Review Board
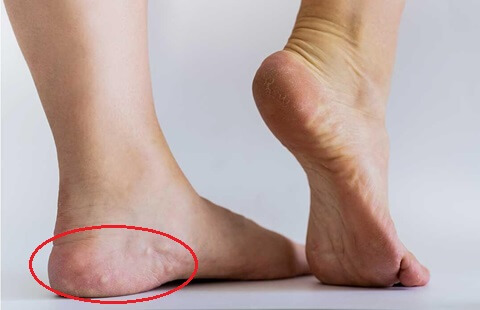
Piezogenic papules are small, soft bumps that can appear on the sides of the feet around the heels. In most cases, they are completely painless and don’t cause any problems.
These papules are typically flesh-coloured or slightly yellowy-white and less than 5mm in diameter.
Around 60-70% of the population may develop piezogenic papules at some point and they are particularly common in people who spend significant periods on their feet, be it standing, walking or playing sports.
The distinctive feature of piezogenic papules is that they become more noticeable when pressure is applied to the feet, such as when standing or walking, and they then disappear when you sit down.
Piezogenic papules can also occur in the wrist, but here we will concentrate on ones in the foot, known as piezogenic pedal papules.
What Are Piezogenic Papules?
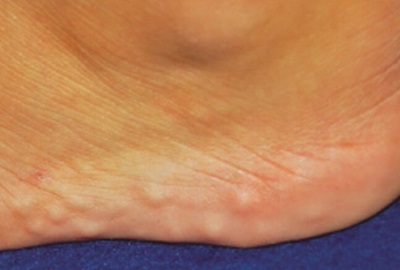
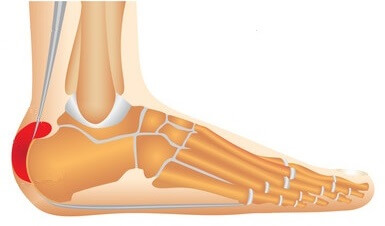
Piezogenic papules are small lumps of fatty tissue that form just underneath the skin on the heels of the feet.
Their development is related to the structure and composition of the foot's connective tissue.
These papules form when subcutaneous fat tissue herniates (protrudes) through defects in the connective tissue into the skin. When pressure is applied to the feet, the fat is forced into these small herniated pockets, creating the characteristic bumps when weight-bearing.
Pedal piezogenic papules are most commonly found along the inner side of the heels, but can also occur at the back and outer side of the heels. They tend to affect both feet, known as bilateral piezogenic papules, rather than just one foot and are the most common cause of small heel lumps.
Piezogenic pedal papules are usually fairly small, ranging in size from approximately 0.2-1cm in diameter. People often have multiple lumps, typically around 2- 5 per foot, but in some cases, there may be up to 20 small lumps.
Piezogenic pedal papules can occur at any ages and have no racial predisposition.
Piezogenic Papules Cause
The exact cause of piezogenic papules is unclear but is thought to be related to a combination of:
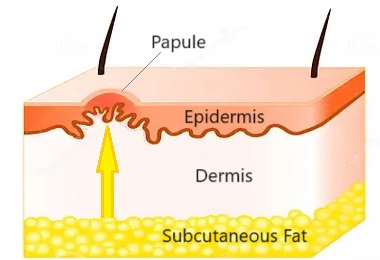
- Connective Tissue Weakness: Connective tissue is a complex network of fibres and cells e.g. collagen and elastic tissue that provides structural support and stability to various structures in the body, e.g. skin, tendons and ligaments. Weakness or laxity in the connective tissue compromises the integrity of the foot dermis (the middle layer of your skin). This creates pockets or spaces where the subcutaneous fat can herniate. Fat tissue pushes through the weakened areas forming small bulges, resulting in the characteristic little bumps underneath the skin.
- Foot Biomechanics: Biomechanical factors, such as abnormalities in foot structure e.g. flat feet, can contribute to the development of piezogenic papules. Excessive pressure on specific areas of the foot due to improper weight distribution can exacerbate the herniation of fat through the weakened connective tissue.
- Activity: People who spend a significant amount of time on their feet, be it standing, walking or running are more prone to developing piezogenic papules. Sports enthusiasts are often affected, particularly long-distance runners, figure skaters or those taking part in high-impact sports. The mechanical stress experienced during weight-bearing activities increases the pressure on the fat pads in the foot and can lead to herniation
- Genetics: while there is no specific known genetic cause for piezogenic pedal papules, there does seem to be a familial link with successive generations in the same family often being affected. Piezogenic lesions are more common in females compared to males
- Medical Conditions: piezogenic papules are more common in people with certain medical conditions, most notably Ehlers-Danlos Syndrome (a connective tissue disorder) and Prader-Willi Syndrome (a complex genetic disorder caused by missing genetic material on chromosome 15). This is thought to be due to the associated collagen weakness with these conditions
- Weight: people with excess weight or obesity are at increased risk of piezogenic papules due to increased pressure on the feet
Common Symptoms
Common symptoms of piezogenic papules are:
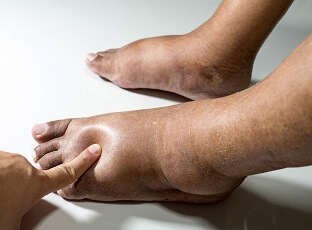
- Bumps: multiple small, flesh-coloured or yellow to white lumps that form in clusters around the heel, particularly the inner side. Most people have bilateral piezogenic papules i.e. lumps on both feet
- Soft: to touch at rest and become firm or tense when weight-bearing
- Painless: in most cases, pedal piezogenic papules are completely painless and don’t cause any symptoms. Occasionally, they may cause some foot pain or discomfort which can limit occupational or sporting activities but this is rare. Pain from piezogenic papules is thought to be related to fat necrosis (cell death) from a lack of adequate blood supply due to compression
- Visible: one of the most prominent features of piezogenic papules are that they tend to only be visible when you are standing or weight-bearing through your heels. They usually disappear completely as soon as you stop putting any weight or pressure through your feet
Diagnosing Piezogenic Papules
In most cases, piezogenic papules can be diagnosed by your health professional with a simple examination. They will ask you about your symptoms, how they started and about any other health conditions and then carry out a physical examination.
Piezogenic papules are typically diagnosed if your foot lumps have the following features:
- Bumps appear when you stand up and resolve when you are non-weight bearing
- Bumps feel firm when you are weight-bearing through your feet
- Small lumps, usually less than 0.5cm diameter, in clusters around the heel
- Lumps are bilateral – on both feet
In some cases, you may be sent for a high-frequency ultrasound to confirm the diagnosis.
There are lots of other possible causes of heel lumps including:
Piezogenic Papules Treatment
In most cases, piezogenic papules treatment is not necessary as they are completely asymptomatic. But on the rare occasions that these foot lumps do cause pain or impede function there are a few treatment options for piezogenic papules:
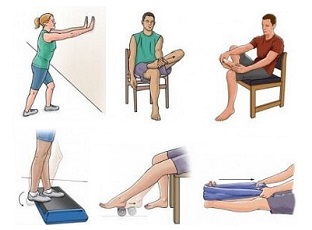
- Avoid Prolonged Weight-Bearing: the best treatment for painful piezogenic papules is to reduce how much time you spend on your feet. This may mean limiting how long you stand or walk for or taking a break from sporting activities
- Footwear: wear wide-fitting shoes with good arch-support and cushioning to help distribute pressure more evenly across the foot
- Orthotics: wearing orthotic inserts in your shoes, such as foam or gel heel cups or medial arch supports can help reduce the pressure on your heels and the piezogenic papules
- Weight-Loss: losing weight if you are over-weight or obese helps to reduce the pressure through your feet and reduce piezogenic papule pain
- Compression Stockings: provide support and reduce swelling
- Injections: intra-lesional injections combining corticosteroid and local anaesthetic can be helpful with painful piezogenic pedal papules, particularly for people with Ehlers-Danlos Syndrome. Some people require two or three injections over a few months for symptoms to fully resolve
- Surgery: if significant symptoms persist despite treatment, your doctor may advise removing piezogenic papules surgically, known as surgical excision, but this is rarely necessary
Pedal Piezogenic Papules Summary
- Piezogenic papules are an extremely common cause of small, flesh-coloured heel lumps.
- They are caused by weakness and laxity in the connective tissue around the heel that allows small amounts of fatty tissue to protrude through, forming small pockets just underneath the surface of the skin.
- Piezogenic pedal papules are typically around 2mm in diameter but can get as large as 1cm.
- The classic feature of piezogenic pedal papules is that they become more noticeable when pressure is applied through the heels, and they disappear when you are non-weight bearing.
- Piezogenic papules are completely harmless and in most cases, don’t cause any pain or discomfort.
- Treatment for symptomatic pedal piezogenic papules usually involves a combination of rest, activity modification and orthotics. In persistent cases, corticosteroid injections or surgery may be advised but this is rare.
You may also be interested in the following articles:
- Heel Lumps
- Heel Pain Causes
- Foot Lumps & Bumps
- Lump On Side Of Foot
- Burning Foot Pain
- Foot Pain Diagnosis Guide
Page Last Updated: 11/23/23
Next Review Due: 11/23/25
Related Articles
References
- National Institutes Of Health: Piezogenic Pedal Papule. F. Brown & C. Cook. August 2023
- AOCD: Piezogenic Papules. American Osteopathic College Of Dermatology
- British Medical Journal (BMJ): Piezogenic Pedal Papules. F. Han 2018