- Home
- Common Foot Problems
- Plantar Fasciitis
Plantar Fasciitis Symptoms
Written By: Chloe Wilson BSc(Hons) Physiotherapy
Reviewed By: FPE Medical Review Board
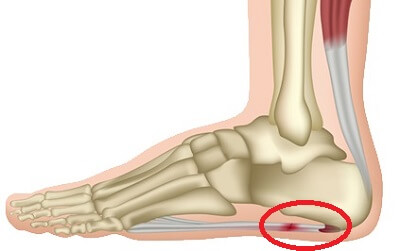
Plantar fasciitis symptoms of pain and tenderness under the heel are a common problem.
Plantar fasciitis is a common cause of foot arch and heel pain and affects approximately 1-in-10 people.
It develops when there is damage and inflammation of the plantar fascia, the thick band of tissue on the sole of your foot.
Plantar fasciitis usually develops due to overuse and is a common problem for runners and people who spend long periods on their feet.
But exactly what is plantar
fasciitis? Here we will look at the causes, symptoms and treatment options as
well as how to prevent this common cause of foot arch pain.
What Is The Plantar Fascia?
The plantar fascia is a thick, tough, fibrous band made up of collagen fibres, which runs along the sole of your foot.
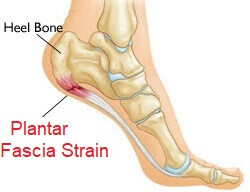
It originates from the heel bone (calcaneus), extends along the bottom of the foot and attaches to the bottom of the toes. It helps to support the arch of your foot and transfers forces across your foot when you walk or run.
There are three parts to the plantar fascia. The central portion is the largest with smaller bands coming out of each side known as the medial and lateral portions.
Plantar fasciitis symptoms develop if too much strain is placed on the plantar fascia, usually from overuse or repetitive actions, causing small tears to develop in the collagen fibres. This results in swelling and inflammation. If the problem continues, it may develop into plantar fasciosis, which means there is chronic degeneration of the tendon rather than inflammation.
Associated Problems
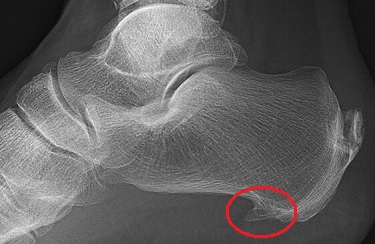
In approximately two-thirds of cases, plantar fasciitis symptoms are accompanied by the presence of a bone spur.
When there is repeated tension on the plantar fascia, it pulls on the
area of bone where the tendon attaches to the heel bone, known as the
calcaneal tubercle.
The body responds by laying done excess bone, known as a heel bone spur, to try and protect itself from injury.
This bone spur then further irritates the plantar fascia making the problem worse.
People often mistakenly think it is the bone spur that causes the plantar fasciitis, but in actual fact, the bone spur develops as a result of the condition.
What Causes Plantar Fasciitis?
Plantar fasciitis symptoms often develop for the following reasons:
- Overuse: Being on your feet for long periods, be it standing, walking or running, especially on hard surfaces
- Foot Biomechanics: Abnormal foot positions such as flat or high foot arches or excessive pronation increase the strain on the plantar fascia
- Muscle Tightness: The plantar fascia is closely linked with the Achilles tendon and calf muscles. Tightness and weakness in the calf therefore predispose the plantar fascia to injury by causing it to repeatedly overstretch
- Weight: Being overweight places more strain through the tendon
- Poor Foot Wear: Wearing shoes that are worn, lack good arch support and cushioning
- Exercise: Suddenly increasing the amount you exercise (frequency or intensity), or changing the surface you exercise on e.g. from track to road
- Age: It most commonly affects people between the ages of forty and sixty
- Gender: Women are twice as likely to suffer from it as men
Plantar Fasciitis Symptoms
The most common of plantar fasciitis symptoms is pain that is worse after rest, either first thing in the morning or after sitting for long periods. In fact, plantar fasciitis is the most common cause of morning foot pain.
This is because the fascia tightens slightly. As you walk around, it then stretches out slightly and symptoms often improve. However, if you are on your feet too much, the plantar fasciitis symptoms return.
Pain from plantar fasciitis is usually felt underneath the heel where the tendon arises from the heel bone, approximately four centimetres forwards from the back of the heel. It is usually tender to touch and there may be a hard lump under foot.
Plantar fasciitis symptoms are often worse when the foot and toes are pulled up (known as dorsiflexion) as this increases the tension on the tendon. Other activities where the plantar fascia is stretched e.g. standing on your tip toes or walking up stairs also tend to increase the pain.
Your doctor can usually diagnose the condition from talking to you about your plantar fasciitis symptoms and examining your foot. Occasionally, they may carry out other tests such as x-rays or ultrasound scan to rule out other causes of pain.
What Is The Best Treatment For Plantar Fasciitis?
Plantar fasciitis treatment usually involves a combination of things including:
- Exercises: to stretch and strengthen the foot
- Ice Packs: to reduce pain and inflammation
- Orthotic Inserts: for shoes that help to support the foot
- Steroid Injections: to reduce pain and inflammation
If conservative treatment fails to resolve the symptoms of plantar fasciitis, then surgery may be recommended.
Studies have shown that the sooner plantar fasciitis treatment is started after symptoms develop, the quicker the recovery process. Plantar fasciitis symptoms usually resolve but they can take months.
You can find out all about how to treat plantar fasciitis and stop it from coming back in the plantar fasciitis treatment section.
Differential Diagnosis
There are a number of other conditions that present with similar symptoms to plantar fasciitis such as:
- Achilles Tendonitis: inflammation & degeneration of the achilles tendon
- Tarsal Tunnel Syndrome: narrowing of one of the nerve passages
- Posterior Tibial Tendonitis: inflammation & degeneration of the posterior tibial tendon
- Heel Pad Syndrome: irritation or thining of the fat pad in the middle of the heel
- Foot Cramps: involuntary spasms in the foot muscles
- Plantar Fibromatosis: nodules form in the plantar fasciia
You can find out more about each of these conditions in the foot arch pain section.
Prevention Strategies
In order to prevent the onset or recurrence of plantar fasciitis symptoms, there are a number of things you can do:
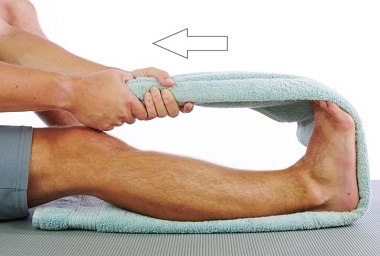
- Stretching Exercises: regularly stretching the calf muscles and plantar fascia is one of the best ways to reduce the chance of developing the condition
- Strengthening Exercises: Strengthening the foot, ankle and calf muscles reduce the chance of developing plantar fasciitis
- Wear Good Footwear: Flat shoes that provide good cushioning and arch support. You may also benefit from orthotic inserts in your shoes
- Lose Weight: But only if you are overweight. Always talk to your doctor before starting any weight loss programmes
- Exercise Appropriately: Avoid over training, particularly if you are just starting out and try and avoid hard surfaces
- Toe Stretchers: Products like the Yoga Toe or Happy Feet Toe Stretcher Socks help to stretch out the muscles and ligaments around the feet and realign the bones. People often find they are a great way to reduce the pain of plantar fasciitis. You can find out more about how they work and read user reviews in the Toe Stretchers section.
What Else Can Help?
You can find out more about the best ways to treat and prevent plantar fasciitis in the plantar fasciitis treatment section including the most effective exercises, which shoe insoles work best, injections and when surgery is indicated.
If these plantar fasciitis symptoms aren't sounding quite like your problem, visit the foot pain diagnosis or foot arch pain sections for help working out what is wrong.
You may also be interested in the following articles:
- Ball Of Foot Pain
- Pain On Side Of Foot
- Nerve Pain In The Foot
- Swollen Feet & Ankles
- Foot Numbness
- Foot Lumps & Bumps
- Morning Foot Pain
- Foot Pain When Walking
Related Articles
Page Last Updated: 27th November, 2025
Next Review Due: 27th November, 2027