- Home
- Common Foot Problems
- Mucous Cysts
Digital Mucous Cyst
Written By: Chloe Wilson BSc(Hons) Physiotherapy
Reviewed By: FPE Medical Review Board
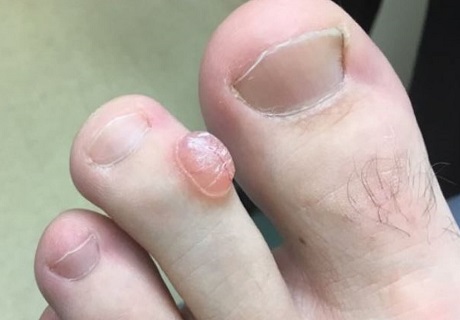
A digital mucous cyst is a small fluid-filled lump that forms on the toes or fingers.
Typically associated with osteoarthritis, mucous cysts often form near a nail and may or may not cause pain.
In most cases, a digital mucoid cyst will settle down on its own in a few weeks, but they often come back.
Here we look at the common causes and symptoms of a digital mucous cyst, how they form, how they are diagnosed and the best treatment options to reduce any symptoms and prevent recurrence.
What Is A Mucous Cyst?
A digital mucous cyst is a benign (i.e. non-cancerous) swelling or growth that occurs in the toes or fingers. They look like small fluid-filled sacs, usually less than 1cm in diameter.
Digital mucous cysts most commonly occur either near the nail or by the joint closest to the nail, known as the distal interphalangeal joint (DIP).
Mucous cysts can also develop in the mouth but here we are going to concentrate on ones that occur in the toes and fingers.
A digital mucous cyst can also be referred to as a digital myxoid cyst, mucoid cyst or muco-cutaneous cyst. Technically, they are pseudo cysts, i.e. fake cysts, as they are not surrounded by a capsule like true cysts are.
What Causes A Digital Mucous Cyst?
The exact cause of a digital myxoid cyst is unclear but is thought to be linked to two possible variations:
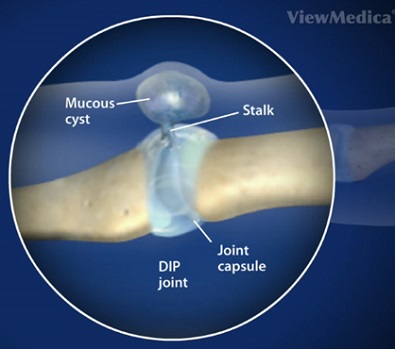
- Synovial Tissue Degeneration: Weakening in the joint capsule and degeneration of the synovial lining allows fluid to seep out of the joint through a "stalk". The fluid pools, forming a small nodule or muco-cutaneous cyst
- Excess Mucin Production: aka focal mucinosis. Abnormal over-production of mucin in fibroblast cells cause mucopolysaccharides to build up in the skin forming a myxoid cyst
Digital mucous cysts are commonly linked with osteoarthritis due to the wear and tear and degeneration in the joint, particularly when osteophytes (bone spurs) are present e.g. with hallux rigidus - big toe arthritis
In some cases, a digital mucous cyst may develop after trauma to the toe or finger – this is most common in the under 30’s.
Digital myxoid cysts are more common in women than men at a rate of around 3:1 and typically affect the dominant hand/foot. There is no obvious genetic or hereditary link with digital myxoid cysts and they are not contagious or cancerous.
Digital mucous cysts are most common in people over the age of 55 due to the link with osteoarthritis. In fact, approximately two thirds of people with osteoarthritis will develop myxoid cysts.
Digital Myxoid Cyst Symptoms
A digital mucous cyst usually develops at the nail or distal joint of a toe or finger and presents as:
- Small, Smooth Lump: digital myxoid cysts are round or oval shaped lumps usually less than 1cm in diameter, most typically 5-8 mm wide
- Skin Coloured: mucous cysts are usually shiny and semi-translucent i.e. slightly see-through. There may be a slightly red or blue tinge if there is some associated bleeding, inflammation or infection in the mucoid cyst
- Tender: myxoid cysts aren’t typically painful but they can be tender to touch. If the mucous cyst is in one of your toes, it may become painful if it rubs against your shoe. When the digital myxoid cyst is linked with osteoarthritis, there may be pain and stiffness in the nearby joint from the arthritis rather than the cyst itself
- Firm Or Rubbery: to touch and dome shaped
- Slow Growing: a digital mucous cyst usually grows slowly over a few months
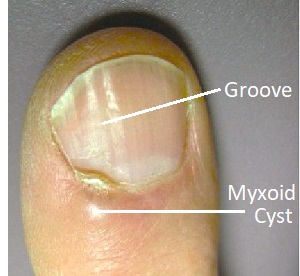
- Split Nail: if the digital mucous cyst is directly under the nail or at the root of the nail, it may cause longitudinal grooves to form under the nail which may then split. In extreme cases this can cause the nail to fall off completely
Occasionally, a digital mucous cyst may burst, releasing thick, jelly-like, sticky fluid that is clear, although in some cases it may be slightly yellowy or tinged with blood. Once the broken skin heals, the myxoid lump usually reappears over time.
Diagnosing Myxoid Cysts

Your doctor can normally diagnose a digital mucous cyst with a simple examination. They will ask you various questions about your symptoms e.g. when they started, how fast the lump has grown etc and will then examine the area.
In some cases, e.g. if the myxoid cyst is directly under the nail or depending on your history, then a biopsy may be performed to confirm the diagnosis and rule out other pathologies. You may also be sent for an x-ray to look for evidence of arthritis or rule out other conditions.
Digital Mucous Cyst Treatment
In many cases, a digital mucous cyst will get better on its own without the need for treatment and there are some things that you can do at home to help:
- Don’t Pop The Cyst: it is really important not to pop or pick at a digital mucous cyst. This can lead to an open would which is prone to infection and permanent scarring, so leave well alone
- Salt Water: If the myxoid cyst does pop, cleaning the area with salt water can help to reduce the risk of infection
- Repetitive Pressure: Pressing firmly over the digital mucous cyst regularly every day for a few weeks can, in some cases, help get rid of the cyst
Further digital mucous cyst treatment is only indicated if the cyst is causing sufficient pain or you are significantly bothered by the appearance of it. In these situations, digital mucous cyst treatment may involve a combination of the following:
1. Aspiration
A digital myxoid cyst may be drained using a sterile needle or knife blade to puncture the skin. This method has a high recurrence rate of up to 50% so the procedure often needs repeating a number of times.
2. Cryotherapy
With cryotherapy, the digital mucous cyst is first drained and then frozen with liquid nitrogen. The lump then falls off.
3. Infrared Coagulation
Infrared coagulation uses heat from infrared radiation to burn away the myxoid cyst at its base. It is a very effective digital mucous cyst treatment options and has one of the lower rates of recurrence – approx. 14-22%.
4. Intralesional Photodynamic Therapy
With intralesional photodynamic therapy, once the digital mucous cyst has been drained, a photosensitizing fluid is injected into the area to make it sensitive to light. The myxoid cyst is then burned off using a laser.
5. Steroid Injection
Another possible digital mucous cyst treatment is steroid injections. The cyst is first drained and then injected with steroid to shrink the cyst. This is often not recommended as it can causing thinning of the skin and has a high recurrence rate of up to 70%.
6. Excision
With an excision, the myxoid cyst and any associated osteophytes (bone outgrowths) in the joint from osteoarthritis are surgically removed. A skin flap or graft will be necessary to cover the incision to reduce the risk of infection. Excision is the most effective treatment for preventing recurrence of a digital mucous cyst
7. Fusion
Joint arthrodesis, where the two bones of the affected joint are fused together, may be recommended for recurrent digital mucous cysts associated with significant osteoarthritis pain
Surgical treatments for digital mucous cysts have high success rates and low recurrence rates, but only tend to be indicated when there is osteoarthritis in the joint or when the myxoid cyst has recurred a number of times. This is because of the potential risks from surgery of scarring, ongoing pain and swelling and the possibility of persistent joint stiffness.
What Else Could It Be?
There are a number of other things that can cause foot lumps. If you think something else might be causing your foot lump rather than a digital mucous cyst, have a look at the following articles
- Foot Lumps & Bumps: common causes of lumps anywhere in your feet
- Lump On Top Of Foot: common causes of lumps and bumps on the top of the your feet and toes
- Lump On Side Of Foot: common causes of lumps and bumps on the sides of your feet and toes
- Lump On Bottom Of Foot: common causes of bumps and lumps underneath your foot and in the arch area
- Swollen Foot Treatment: best ways to reduce foot swelling
- Toe Pain: common causes of toe pain & how to treat them
Summary
Digital mucous cysts are small, fluid filled lumps that form on the toes and fingers. They are usual round or oval shaped and occur at the ends of the digits, usually near the nail.
They are also known as mucoid cysts, muco-cutaneous cysts and digital myxoid cysts.
You should never pop or pick at a digital mucous cyst as it can adversely affect the healing process and increase the infection risk.
In most cases, digital myxoid cysts are harmless, painless and don’t require any treatment, settling down on their own within a few weeks, but they have a high recurrence rate.
There are a number of treatment options for digital mucous cysts including draining the cyst, burning it off and removing the cyst surgically.
If you suspect you may have a digital mucous cyst, get checked out by your doctor.
You may also be interested in the following articles:
- Pain On Top Of The Foot
- Burning Foot Pain
- Foot Swelling & How To Treat It
- Foot Rashes
- Foot & Ankle Anatomy
Related Articles
Page Last Updated: 14th November, 2024
Next Review Due: 14th November, 2026